Simulating Success: Assessing the Impact of Obstetrics Skills Workshop in Enhancing Medical Student Interest and Engagement
BACKGROUND
Obstetric skills are essential for primary care physicians, and early exposure in medical training is associated with greater comfort and likelihood of including obstetrics in future practice.1 Opportunities for medical students to gain hands-on experience are decreasing largely due to reduced patient access, medico-legal constraints, and shifting clinical responsibilities.2 Simulation-based training (ALSO, PROMOTE) is widely used in residency programs and effectively improves confidence and skills in obstetric emergencies and procedures, but comparable opportunities at the medical student level are limited.3-4 This study evaluates the impact of a novel obstetrics skills workshop designed specifically for medical students.
METHODS
A 2.5-hour workshop was offered to 38 first-, second-, and third-year medical students through specialty interest groups with IRB approval (H-57034). The workshop consisted of six simulation-based stations: (1A) fetal non-stress test (NST) case-based interpretation, (1B) laceration repair using a beef tongue model, (1C) cervical assessment using a citrus fruit model, (1D) postpartum hemorrhage estimated blood loss simulation, (1E) obstetric ultrasonography using the SonoSim platform, and (1F) labor procedures including fetal scalp electrode placement, amniotomy, and intrauterine pressure catheter placement performed on a foam-and-balloon model (Figure 1).
Participants completed pre- and post-workshop surveys evaluating both objective knowledge and self-reported proficiency. Objective knowledge was assessed using a six-question test administered at the beginning of the workshop and repeated at its conclusion. The assessment was designed to evaluate knowledge gained during the workshop, with each question corresponding to content covered at one of the simulation stations. For the purpose of analysis, each question was weighted equally with the participants earning one point for each question answered correctly. Proficiency ratings were assessed on 5-point Likert scales, with students rating prior experience before the workshop (1 = no experience to 5 = able to perform independently) and comfort level afterward (1 = very uncomfortable to 5 = proficient). Additionally, general feedback was collected at the end of the workshop.

RESULTS
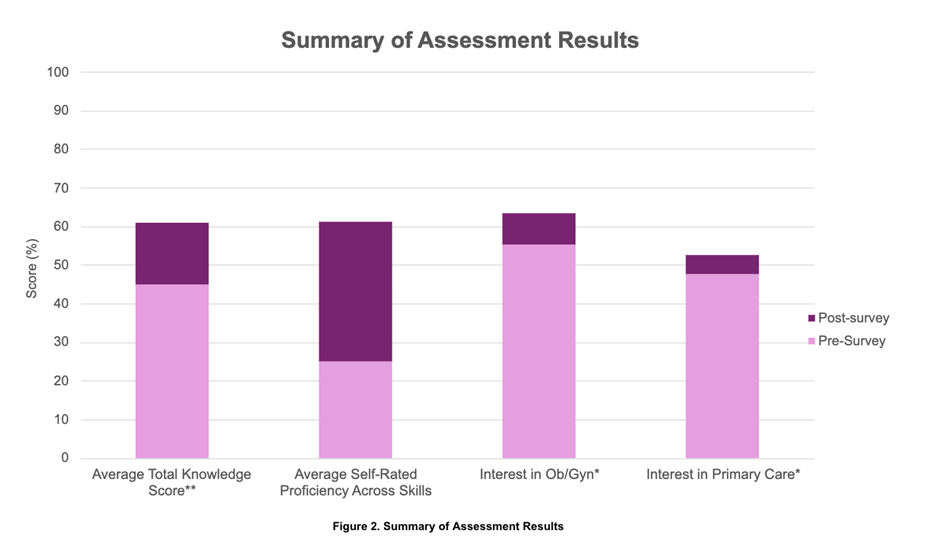
Among 38 participants, 52.6% were first-year, 39.5% second-year, 5.3% third-year, and 2.6% fourth-year medical students. Average objective knowledge scores improved from a mean of 2.59/6 to 3.66/6 (p=0.0008). Average self-reported proficiency increased from 1.67 to 3.52 on a 5-point scale (111% increase relative to baseline), with largest gains observed in amniotomy and ultrasound. Interest in pursuing obstetrics and gynecology as a specialty increased (p = 0.03), along with enthusiasm for primary care in general, including family medicine and obstetrics and gynecology (p = 0.017) (Figure 2). Post-survey results showed 95.7% of students agreed that the workshop increased confidence and comfort with obstetric procedural skills.
DISCUSSION
This study demonstrates that a simulation-based workshop can be effectively utilized to address limitations in early exposure to obstetrics skills among medical student education. The workshop was effective in improving knowledge and self-reported proficiency, with the greatest gains in ultrasound and amniotomy – procedures rarely encountered by medical students outside of structured training. These findings align with prior literature indicating that simulation-based learning fosters engagement and exposure to clinical skills, particularly when access to real patient encounters is limited. This is particularly important given variability in patient volume, clinical teaching opportunities, and access to advanced simulation centers across medical schools. Additionally, students reported increased enthusiasm for obstetrics and gynecology as a specialty and in incorporating these skills into other primary care fields, including family medicine. This suggests that early exposure may play an influential role in shaping the pipeline of future providers in obstetric care. Finally, the workshop’s low cost, brief duration, and adaptable format further support its scalability across diverse educational environments. Several limitations should be noted. First, the study sample size was modest and limited to one institution, which may affect generalizability. Second, outcomes were measured immediately post-intervention; thus, long-term retention of skills and knowledge remains unknown. Future studies should incorporate longitudinal assessments to examine whether early simulation exposure translates to improved residency performance and increased recruitment into primary care.
CONCLUSION
Our findings highlight the value of simulation-based workshops designed specifically for medical students. Integrating such sessions into preclinical and early clinical curricula has the potential to address declining opportunities for obstetric exposure, enhance learner preparedness, and encourage greater interest in primary care specialties that incorporate obstetrics.
REFERENCES
- Pearson J, Westra R. Early Course in Obstetrics Increases Likelihood of Practice Including Obstetrics. Fam Med. 016;48(9):720-724.
- Everett EN, Forstein DA, Bliss S, et al. To the Point: The expanding role of simulation in obstetrics and gynecology medical student education. Am J Obstet Gynecol. 2019;220(2):129-141. doi:10.1016/j.ajog.2018.10.029
- Cohn JD, Kearney MD, Donze ML, O'Brien CS, DeMarco MP. PROMOTE: An Innovative Curriculum to Enhance the Maternity Care Workforce. Fam Med. 2024;56(9):567-571. doi:10.22454/FamMed.2024.146382
- Taylor HA, Kiser WR. Reported comfort with obstetrical emergencies before and after participation in the advanced life support in obstetrics course. Fam Med. 1998;30(2):103-107
